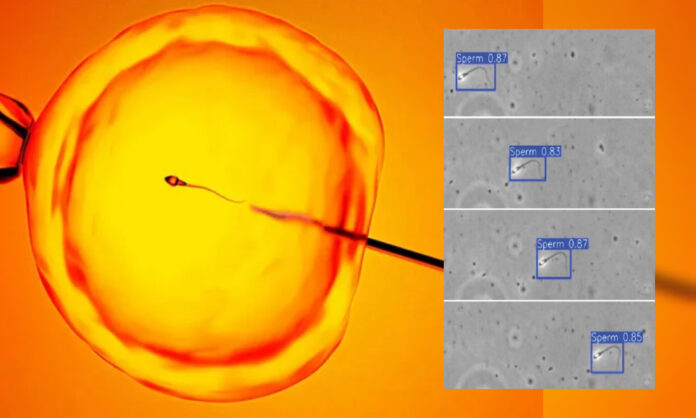
A research team at the Columbia University Fertility Center has developed an artificial intelligence system that can detect extremely rare sperm cells in men previously diagnosed with infertility.
The method is known as the STAR (Sperm Track and Recovery) system and is now being used in clinical settings, contributing to confirmed pregnancies and births.
The technology was developed over a period of about five years, with initial work beginning around 2020.
The system is designed for men with azoospermia, a condition in which no sperm is detected using standard laboratory techniques. While these patients are often told they cannot produce sperm, some may still have very small numbers of viable cells that are difficult to find.
According to Zev Williams, director of the center, the STAR system can detect sperm cells that are missed by conventional methods. “It’s just finding something where we couldn’t see it before,” he said.
How does the system works?
The STAR platform combines imaging, machine learning, and microfluidic engineering:
- Samples flow through channels etched into microfluidic chips
- An imaging system captures approximately 300 frames per second
- A trained AI model analyzes the images in real time
- When a sperm cell is detected, a robotic system isolates it within milliseconds
The approach avoids centrifugation, a standard technique that can damage fragile cells.
Williams reported that, in laboratory testing, the system achieved 100% sensitivity, meaning it can detect a sperm cell if even one is present in the scanned sample.
The technology has been tested in 175 patients who had previously been told they had no chance of producing usable sperm. According to the research team:
- Sperm was identified in just under 30% of cases
- The system detected up to 40 times more sperm than manual searches by trained technicians
One reported case involved a patient with Klinefelter syndrome, a condition associated with reduced or absent sperm production.
After hormone treatment, doctors performed a surgical extraction of testicular tissue. The sample was analyzed using the STAR system, which identified eight viable sperm cells. These were used in in vitro fertilisation (IVF).
The patient’s partner became pregnant in late 2025. The couple is expecting a child in July 2026. A separate case resulted in the birth of a child in 2025, described by the research team as the first birth using this method.
External specialists have noted the potential of the technology but advise caution.
Siobhan Quenby of the University of Warwick said: “One successful pregnancy is an important start. However, further research on more patients is needed before the value of this new treatment can be fully assessed.”
She also noted that patients undergoing long fertility treatments may be vulnerable to high-cost interventions with limited evidence.
Male infertility contributes to approximately 50% of infertility cases, and azoospermia affects about 1% of all men.
Image Credit: The Star System